
Sutherland Shire’s home of TMJ Disorder Remediation
If you suffer from jaw pain, headaches, clicking in your jaw, or facial tension, you may be experiencing TMJ disorder — a common but often misunderstood condition affecting the jaw joints and surrounding muscles.
At our practice, we take a comprehensive, evidence-based approach to diagnosing and treating TMJ disorders, helping patients regain comfort, function and quality of life.
What Is TMJ Disorder?
The temporomandibular joints (TMJs) connect your lower jaw (mandible) to your skull. These joints sit just in front of each ear and allow you to chew, speak, yawn and swallow.
TMJ disorder (TMD) refers to dysfunction, inflammation or structural imbalance affecting:
The jaw joint itself
The surrounding muscles (myofascial pain)
The joint disc (internal derangement)
The bite and occlusion
Because the TMJ is one of the most complex joints in the body, even minor imbalances can lead to significant symptoms.

Common Signs and Symptoms of TMJ Disorder
TMJ symptoms can vary widely. Many patients are unaware that their daily discomfort is jaw-related.
Jaw-Related Symptoms
Clicking, popping or grinding sounds
Jaw pain or tenderness
Limited mouth opening or jaw locking
Difficulty chewing
Uneven bite sensation
Head, Neck and Facial Symptoms
Chronic headaches or migraines
Ear pain or fullness (without infection)
Ringing in the ears (tinnitus)
Facial muscle tension
Neck and shoulder pain
Dental and Bite Changes
Worn, cracked or chipped teeth (including fillings)
Tooth sensitivity
Bruxism (teeth grinding or clenching)
Shifting bite over time
If left untreated, TMJ dysfunction can progress, leading to chronic pain, worsening joint damage and long-term dental complications.

What Causes TMJ Disorder?
TMJ disorder is typically multifactorial. Common contributing factors include:
Chronic clenching or grinding (often stress-related)
Bite imbalance or malocclusion
Trauma to the jaw
Arthritis in the joint
Disc displacement
Poor posture (especially forward head posture)
Sleep-related breathing disorders
In many adults between 25–55 years of age, lifestyle stress and parafunctional habits are major contributors.
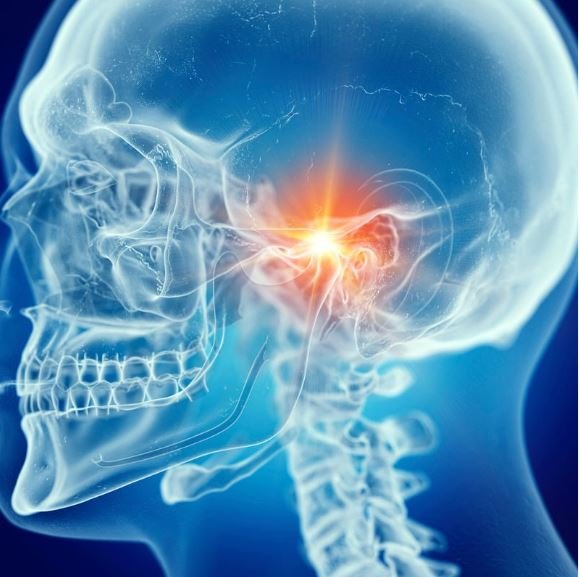
How TMJ Disorder Is Diagnosed
Accurate diagnosis is essential. TMJ pain is frequently misdiagnosed as migraines, sinus issues or ear infections.
A comprehensive TMJ assessment should include:
Detailed symptom history
Jaw movement analysis
Palpation of joint and muscles
Bite and occlusal evaluation
Assessment of wear patterns
Digital imaging (CBCT, TMJ-specific or panoramic radiography when indicated)
In complex cases, advanced imaging such as MRI may be required to evaluate disc position and joint health.
Correct diagnosis determines whether the problem is primarily muscular, joint-related, bite-related, or a combination.

Why Early Treatment Matters
TMJ disorder rarely resolves permanently without addressing the underlying cause.
Delaying treatment can lead to:
Progressive joint degeneration
Chronic facial pain
Worsening headaches
Increased dental wear and tooth structure deterioration
Reduced quality of life
Early intervention is typically simpler, more conservative and more predictable.
Evidence-Based TMJ Treatment Options
Treatment depends on the underlying cause. A structured, conservative-first approach is recommended for the vast majority of our clients. Some options include but are not limited to:
1. Occlusal Splints (Night Guards)
Custom-made splints reduce muscle hyperactivity, protect teeth from grinding, and stabilise the joint.
2. Bite Correction and Occlusal Therapy
If malocclusion is contributing, selective adjustment or orthodontic alignment may improve joint stability.
3. Muscle Relaxation and Pain Management
This may include:
Jaw physiotherapy
Trigger point therapy
Targeted muscle relaxant therapy (TMJ Muscle Injectables)
Anti-inflammatory strategies
4. Orthodontics
Correcting misalignment can reduce strain on the TMJ when appropriately planned.
5. Minimally Invasive Aesthetic Rehabilitation
In patients with severe tooth wear from bruxism, restoring lost vertical dimension can significantly reduce joint strain.
6. Multidisciplinary Care
Complex cases may involve collaboration with:
Physiotherapists
Sleep physicians
ENT specialists
Pain specialists
Surgery is rarely required and is reserved for advanced structural damage of the TMJ joint.

The Emotional and Functional Impact of TMJ Disorder
Chronic jaw pain does not just affect chewing — it affects:
Sleep quality
Work productivity
Confidence in social situations
Mood and stress levels
Relationships
Diet and Nutritional Quality
Many patients describe a constant low-grade tension that becomes part of daily life. It does not have to be that way.
Are You Experiencing TMJ Symptoms?
You may benefit from a professional assessment if you:
Wake up with jaw soreness
Experience frequent tension headaches
Notice clicking or locking of your jaw
Have worn or fractured teeth
Feel your bite has changed
A thorough TMJ consultation can provide clarity, direction and a structured treatment plan tailored to your needs.
Enquire with us Today
Take the First Step Toward Relief
TMJ disorder is treatable. With accurate diagnosis and a personalised treatment approach, most patients experience significant improvement in comfort and function.
If you suspect you may have TMJ disorder, seeking early assessment can prevent long-term complications and restore balance to your jaw, muscles and bite.
Your comfort, function and long-term oral health deserve careful, expert attention.
